 “The DSM helps psychiatrists and psychologists better identify and diagnose mental disorders. Tom M Johnson/Getty Images
“The DSM helps psychiatrists and psychologists better identify and diagnose mental disorders. Tom M Johnson/Getty Images
Before the 1970s, homosexuality was often considered a mental illness. Indeed, the American Psychiatric Association (APA) classified it as such in its first Diagnostic and Statistical Manual of Mental Disorders (DSM), published in 1952. This was not a controversial position at the time — it held with prevailing norms. But then gay activists started protesting at annual meetings of the APA, and presented scientific evidence opposing this view.
In 1973, it was put to the vote and the majority (58 percent) of APA members agreed homosexuality should no longer be considered a mental disorder [source: Group for the Advancement of Psychiatry]. This change was a huge step for gay rights and helped to shift societal thinking on homosexuality. It also demonstrated the power of the DSM, the diagnostic manual of the APA, on public opinion.
Now in its fifth edition and known as DSM-5 (this is the first edition without a Roman numeral), the publication does not offer treatment or medication advice for the 157 disorders described in its pages. Rather, it was designed to help healthcare professionals better identify and diagnose mental disorders, such as those that impact personality, cognition, mood and identity. The manual also provides uniform diagnostic codes for each issue, which are used to facilitate billing and data collection [source: APA]. Often, if a condition is not listed in the DSM, U.S. health insurance companies won’t pay for treatment for it.
The manual is primarily used in the United States, with much of the rest of the world’s health professionals turning instead to the World Health Organization’s (WHO) International Classification of Diseases (ICD), which covers all diseases, not just those psychiatric in nature. APA encourages healthcare professionals to consider DSM-5 and ICD as "companion publications," designed to be compatible with each other.
So how did it start? The DSM was developed in response to an obvious need for mental illness classification systems. The U.S. Census of 1840 took baby steps toward the eventual development of the manual when it added incidents of "idiocy/insanity" to its survey. This was possibly the first attempt at statistical information-gathering related to mental illness, and therefore a pretty big deal. In 1880, the Census fleshed out the mental health categories to include issues like dementia, melancholia, epilepsy and mania [source: APA].
Mental institutions of the past have been the stuff of horror movies, a fate sometimes worse than death for those who wound up behind their walls. Just a century ago, people were institutionalized for relatively common, now-treatable problems, like bipolar disorder [source: Mental Health America]. Fortunately, mental illness detection, treatment and diagnosis, although still far from perfect, have come a long way. One of the measures credited with improving care quality was the development of the DSM.
In 1917, the American Medico-Psychological Association (the forerunner of the APA) and the National Commission on Mental Hygiene came up with a plan, adopted by the Census Bureau, for gathering uniform health statistics in mental hospitals. And in 1921 the APA started to develop psychiatric classifications for various severe psychiatric disorders. After World War II, the APA used a bigger classification system developed by the U.S. Army as it was treating veterans to develop the first DSM [source: APA].
Contents
- The DSM Classification Process
- Changes from DSM-IV to DSM-5
- The Addition of Section III
- Controversies and Reversals With the DSM
The DSM Classification Process
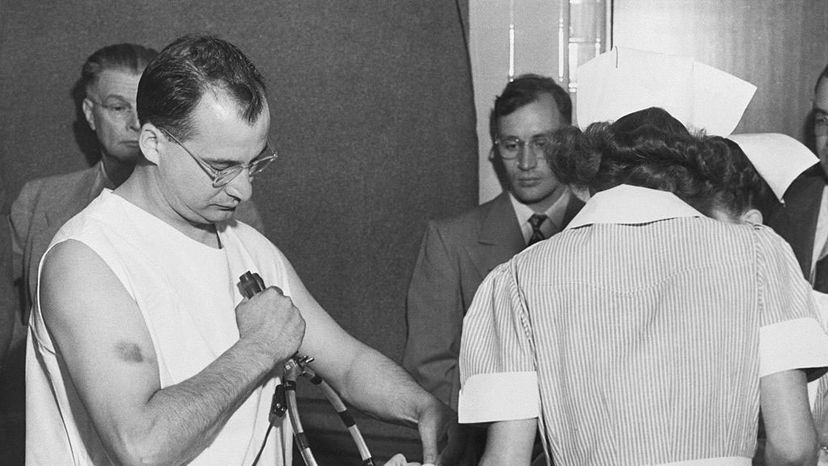 “Dr. James G. Shanklin, a hospital psychiatrist, administers electric shock and anesthesia to a patient in 1949. The DSM was originally developed to catalog psychiatric disorders at a time when mentally ill people received poor or no treatment. Bettman/Getty Images
“Dr. James G. Shanklin, a hospital psychiatrist, administers electric shock and anesthesia to a patient in 1949. The DSM was originally developed to catalog psychiatric disorders at a time when mentally ill people received poor or no treatment. Bettman/Getty Images
The first official version of the DSM was released in 1952, with the most recent version — DSM-5 — published in 2013 [sources: Kawa and Giordano, APA]. Each update was the result of years of DSM-5 Task Force meetings, discussion by work groups and input by many psychiatric experts around the world. Today, the manual includes a trio of components for each disorder:
Diagnostic classification contains the list of mental disorders officially recognized. All diagnoses are assigned a diagnostic code (obtained from the World Health Organization’s ICD), which is helpful for collection of data, as well as streamlining the billing process for providers and medical institutions.
Diagnostic criteria are also available for every disorder. The criteria lists symptoms, including their duration, that must be present to achieve a particular diagnosis. There are also a litany of other disorders and symptoms listed that should first be ruled out.
Descriptive text for each disorder contains information about prevalence, development and course, risk and prognostic factors, and other relevant information.
It’s no small feat for a mental illness to be added to the DSM. In fact, DSM-IV wasn’t all that different from DSM-5, but the changes that did make the cut were thoroughly reviewed and discussed by some of the foremost minds in the psychiatric field. DSM-IV was published in 1994, so the DSM-5 Task Force had to review all scientific studies published on psychiatric disorders since then. Remember, DSM-5 wasn’t published until 2013, so that’s nearly 20 years’ worth of research to look at.
Following the comprehensive review, proposals to modify existing diagnoses were made, which required vigorous discussion and debate among the committee members, plus input from outside experts. All proposals were examined by the task force, as well as two additional committees created for a more independent-opinion, the Scientific Review Committee and a Clinical and Public Health Committee [source: APA].
New editing changes have streamlined the process, however. Rather than waiting decades between issues, experts can now submit changes online, helping to make the manual more timely and current. Once approved by the APA board of trustees, clinicians and other DSM users are notified about the edit, so they can make diagnosis changes in real time.
"This has been a major advance," says Dr. Philip Wang, director of the APA’s research division, which supervises the DSM. He says this change has effectively turned DSM-5 into a "living document," of sorts. "Let’s say there is enough scientific evidence and let’s say there is a valid change, to have to wait 15 or 20 years for clinicians and patients to benefit from that change is unconscionable," he adds.
Once a change is made, users can hover over it in the online version to find out the pertinent details, what the previous material was, and the supporting scientific evidence that inspired the edit. "It’s completely transparent, continuous, and at the end of the day, it hopefully is good for clinicians and benefits patients," Wang says.
Changes from DSM-IV to DSM-5
 “David Moloney, an adult with Asperger’s syndrome poses for a photo in 2013 after sharing his concerns about the fact that his diagnosis would be gone from the new DSM-5 and folded into a diagnosis of Autism Spectrum Disorder. Tara Walton/Toronto Star via Getty Images
“David Moloney, an adult with Asperger’s syndrome poses for a photo in 2013 after sharing his concerns about the fact that his diagnosis would be gone from the new DSM-5 and folded into a diagnosis of Autism Spectrum Disorder. Tara Walton/Toronto Star via Getty Images
One of the major overhauls between DSM-IV to DSM-5 was done to handle the problem of excessive comorbidity, which is when one patient is diagnosed with two or more conditions. There was a lot of this going on with DSM-IV and earlier versions. "If someone was diagnosed with one condition they were likely to also be [incorrectly] diagnosed with having a second condition," Wang explains. "A lot of patients would fall in between categories, and there was a lot of use of a category called ‘not otherwise specified’ [NOS]. If you have that kind of comorbidity and that kind of use of NOS, it means that the categories are not quite working for patients and clinicians."
To address this problem, which clinicians had reported for many years previously, the DSM-5 combined nearly 30 disorders, effectively reducing diagnoses, comorbidity and unhelpful NOS. Two diagnoses were eliminated entirely, and 15 were added, according to Wang.
Probably the most well-known diagnosis removed was Asperger’s syndrome, which is now classified under the autism spectrum disorder (ASD) diagnosis. This change was made in response to the research and clinical findings gleaned over the course of the previous couple of decades, with autism spectrum disorder revised to encompass four previously distinguished disorders (autistic disorder, Asperger’s disorder, childhood disintegrative disorder and pervasive developmental disorder not otherwise specified) [source: Autism Society].
The hope is that refining the criteria and including a severity scale will make a diagnosis more valid and reliable. However, some critics expressed concern that removing a long-held diagnosis would negatively affect patients and their families and cause confusion in the billing/treatment communities [source: Autism Research Institute].
"I know that there was a lot of deliberation about it and then a lot of questioning," Wang explains of the switch. "It’s something that people are still wrestling with." However, the advocacy group Autism Speaks points out that there should not be any change in accessing services or insurance coverage if someone’s diagnosis was formerly Asperger’s and is now ASD.
DSM-5 has also revamped disorders into a lifespan approach. Instead of classifying certain issues as solely "childhood disorders," it discusses how they change and manifest at all stages. DSM-5 also emphasizes the importance of parents in diagnosis and treatment. Also, although many disorders were streamlined, two childhood-specific issues were added.
Disruptive mood dysregulation disorder (DMDD) describes severe, recurrent outbursts of temper that are extremely inappropriate for the situation or in level of intensity. And social communication disorder (SCD) is "characterized by a persistent difficulty with verbal and nonverbal communication that cannot be explained by low cognitive ability," according to the APA. Prior editions of DSM didn’t include the appropriate treatment for these problems because they had not been completely defined and studied, and as such treatment varied and suffered [source: APA: DSM-5 and Diagnoses for Children Fact Sheet].
The Addition of Section III
DSM-5 also introduced Section III, which is for conditions where there is not enough scientific data yet to determine whether they should be classified as psychiatric disorders. Among these conditions are Internet Gaming Disorder, Caffeine Use Disorder (see sidebar) and Persistent Complex Bereavement Disorder [source: APA].
Section III also contains measures and models that have potential to help clinicians better evaluate patients. "There’s been a push that there are dimensions that run across disorders," Wang says. "Some patients have symptoms or signs that appear across many diagnostic categories. That’s why they’re ending up with lot of comorbid diagnoses."
So, the DSM-5 introduced the cross-cutting dimensional measure, which helps clinicians determine if there are underlying dimensions that could be present in multiple disorders. Although this approach is still in need of validation before it can be permanently included in the main DSM-5, Wang notes that many physicians already follow this line of thought. "It’s like when primary care doctors do a review of systems," he explains. "They probe further if there’s a positive. In mental health we need a mental health review of systems. That’s what the DSM cross-cutting measure is."
Section III also includes a cultural formulation interview guide, with questions to help clinicians identify how a patient’s cultural background affects their perception and presentation of psychiatric symptoms, treatment and diagnosis. "The interview provides an opportunity for individuals to define their distress in their own words and then relate this to how others, who may not share their culture, see their problems. This gives the clinician a more complete foundation on which to base both diagnosis and care," APA explains in a Section III Fact Sheet.
Caffeine Use Disorder (CUD) is a Thing
One or two cups of Joe is no big deal, but too much caffeine can actually result in "caffeine intoxication," which can even land a person in the hospital. DSM-5 added CUD to Section III as a possible diagnosis for further study. Until research either confirms or denies this diagnosis, stop to consider the following: Do you really want to quit caffeine use, or at least control it, but are unsuccessful? Do you continue to use caffeine even if you know it causes you physical or psychological issues? Do you experience excessive withdrawal if you do try to back off usage? If you answered yes to all three you could be a candidate for CUD [source: Addicott].
Controversies and Reversals With the DSM
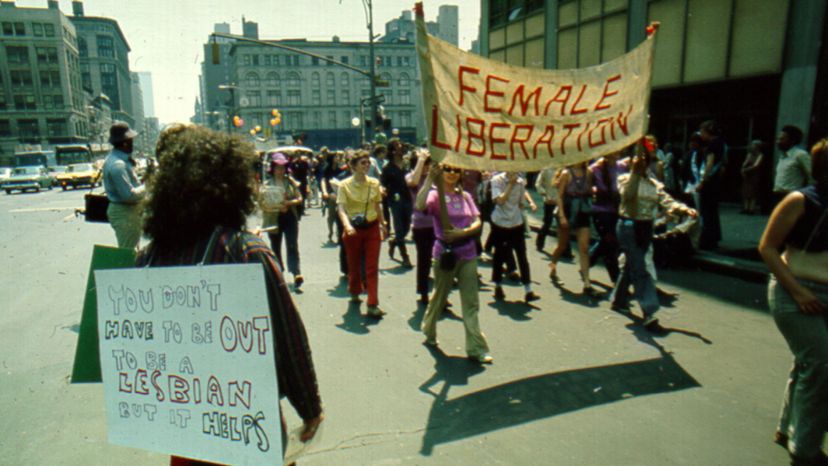 “Gay and lesbian activists protest discrimination during the Christopher Street Liberation Day March, June 1971 in New York. At the time, the DSM still classified homosexuality as a mental disorder. Michael Ochs Archives/Getty Images
“Gay and lesbian activists protest discrimination during the Christopher Street Liberation Day March, June 1971 in New York. At the time, the DSM still classified homosexuality as a mental disorder. Michael Ochs Archives/Getty Images
Some key about-faces are proof that the DSM isn’t opposed to changing with the times. Here are some examples of major turnarounds:
Consenting adults who enjoy relatively unconventional BDSM, fetishes or even cross-dressing need not fear being considered mentally ill, thanks to the DSM-5 update, which "depathologized" kinky sex. Instead, they are now considered people with "unusual sexual interests" [source: National Coalition for Sexual Freedom].
Also, in keeping with the greater acceptance of transgender people, DSM-5 replaced the diagnosis of "gender identity disorder" with the less controversial "gender dysphoria," which does not classify those who don’t identify with their birth gender as having a mental disorder. However, the diagnosis does spell out some of the challenges of living with gender dysphoria, as well as the different paths people choose to take to resolve this [source: APA]. (Some critics of the change point out that some insurance companies won’t cover hormonal or surgical treatment if the condition is not considered a mental disorder.)
Another big change was the removal of homosexuality as a mental disorder from DSM-II. "APA’s 1973 diagnostic revision was the beginning of the end of organized medicine’s official participation in the social stigmatization of homosexuality," writes Jack Drescher in the journal Behavioral Sciences. "Similar shifts gradually took place in the international mental health community as well. In 1990, the World Health Organization removed homosexuality per se from the International Classification of Diseases (ICD-10). "
This was all accomplished in baby steps. Initially, DSM-III made a distinction between people who were comfortable with their homosexuality and those who weren’t — the latter could be diagnosed with the mental disorder Sexual Orientation Disturbance. Eventually, this diagnosis was also removed from the manual in the 1980s [source: Group for the Advancement of Psychiatry].
One complaint about the DSM is that once a condition is included in the manual, it may turn what once was considered "normal" behavior into a pathological illness that must be treated — often with medication. "Many millions of people with normal grief, gluttony, distractibility, worries, reactions to stress, the temper tantrums of childhood, the forgetting of old age, and ‘behavioral addictions’ will soon be mislabeled as psychiatrically sick and given inappropriate treatment," wrote psychiatrist Allen J. Frances in Psychology Today at the time that DSM-5 was going to press.
But Wang points out that DSM-5 has incorporated an acuity measure to help with that, since so many disorders range widely in their severity. These scales help clinicians better evaluate symptoms and levels of impairment. For example, let’s say you’re grieving over the death of your father. Are you still able to cope with life or are you barely able to get out of bed? Once assessed, clinicians will be better able to land on the appropriate treatment, whether medication, watchful waiting, talk therapy or a combination of these [source: APA Integrated Assessment fact sheet].
Lots More Information
Author’s Note: How the DSM (Diagnostic and Statistical Manual of Mental Disorders) Works
The human mind is marvelous, but for some can be a terrible trap of sorrow, anxiety and a million other emotions. People dealing with mental illness (not to mention the loved ones who support them) deserve an up-to-date, fully considered guide to help them and their clinicians provide the best support possible. Let’s hope the DSM continues to strive for these noble goals.
Related Articles
- Is it possible to share your psychosis?
- Can TV viewing cause autism?
- How Schizophrenia Works
- How PTSD Works
- Do We Really Need Internet Addiction Treatment Centers?
More Great Links
- DSM-5
- This American Life: 81 Words
Sources
- Addicott, Merideth A. "Caffeine Use Disorder: A Review of the Evidence and Future Implications." Current Addiction Reports. Sept. 2014 (Sept. 17, 2017) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4115451/
- American Psychiatric Association. "About DSM-5." 2017 (Sept. 10, 2017) https://www.psychiatry.org/psychiatrists/practice/dsm/about-dsm
- American Psychiatric Association. "DSM History." 2017 (Sept. 10, 2017) https://www.psychiatry.org/psychiatrists/practice/dsm/history-of-the-dsm
- American Psychiatric Association. "DSM-5 and Diagnoses for Children Fact Sheet." 2017 (Sept. 15, 2017) https://www.psychiatry.org/psychiatrists/practice/dsm/educational-resources/dsm-5-fact-sheets
- American Psychiatric Association. "DSM-5: Frequently Asked Questions." 2017 (Sept. 10, 2017) https://www.psychiatry.org/psychiatrists/practice/dsm/feedback-and-questions/frequently-asked-questions
- American Psychiatric Association. "ICD vs. DSM." 2017 (Sept. 10, 2017) http://www.apa.org/monitor/2009/10/icd-dsm.aspx
- American Psychiatric Association. "Integrated Assessment Fact Sheet." 2017 (Sept. 15, 2017) https://www.psychiatry.org/psychiatrists/practice/dsm/educational-resources/dsm-5-fact-sheets
- American Psychiatric Association. "Making a Case for New Disorders." 2017 (Sept. 10, 2017) https://www.psychiatry.org/File%20Library/Psychiatrists/Practice/DSM/APA_DSM-5-Making-Case-for-New-Disorders.pdf
- American Psychiatric Association. "Section III Fact Sheet." 2017 (Sept. 15, 2017) https://www.psychiatry.org/psychiatrists/practice/dsm/educational-resources/dsm-5-fact-sheets
- American Psychiatric Association. "What is Gender Dysphoria?" 2017 (Oct. 2, 2017) https://www.psychiatry.org/patients-families/gender-dysphoria/what-is-gender-dysphoria
- Autism Research Institute. "Updates to the APA in DSM-V – What do the Changes Mean to Families Living with Autism?" 2017 (Oct. 2, 2017) https://www.autism.com/news_dsmV
- Autism Society. "Asperger’s Syndrome." 2017 (Sept. 15, 2017) http://www.autism-society.org/what-is/aspergers-syndrome/
- Centers for Disease Control and Prevention. "Mental Health Basics." 2017 (Sept. 10, 2017) https://www.cdc.gov/mentalhealth/basics.htm
- Drescher, Jack. "Out of DSM: Depathologizing Homosexuality." Behavioral Sciences. Dec. 2015 (Sept. 17, 2017) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4695779/
- Frances, Allen J. M.D. "DSM-5 is Guide Not Bible – Ignore Its 10 Worst Changes." Psychology Today. Dec. 2, 2012 (Sept. 17, 2017) https://www.psychologytoday.com/blog/dsm5-in-distress/201212/dsm-5-is-guide-not-bible-ignore-its-ten-worst-changes
- Group for the Advancement of Psychiatry. "The History of Psychiatry and Homosexuality." (Oct. 6, 2017) http://www.aglp.org/gap/1_history/
- Kawa, Shadia and James Giordano. "A brief historicity of the Diagnostic and Statistical Manual of Mental Disorders: Issues and implications for the future of psychiatric canon and practice." Philosophy, Ethics and Humanities in Medicine. Jan. 13, 2012 (Sept. 10, 2017) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3282636/
- Mental Health America. "Our History." 2017 (Sept. 10, 2017) http://www.mentalhealthamerica.net/our-history
- National Coalition for Sexual Freedom. "The DSM Says Kink is OK!" 2017 (Sept. 17, 2017) https://www.ncsfreedom.org/key-programs/dsm-v-revision-project/dsm-v-program-page
- Wang, Philip, M.D., PhD. American Psychiatric Association. Telephone interview, Sept. 10, 2017.
- World Health Organization. "ICD-10." 2017 (Sept. 10, 2017) http://www.who.int/classifications/icd/en/

